Plantar fasciitis: why your summer shoes may be making it worse
Experts explain plantar fasciitis, along with 7 ways to ease the pain – and how your most comfortable shoes may not be helping.
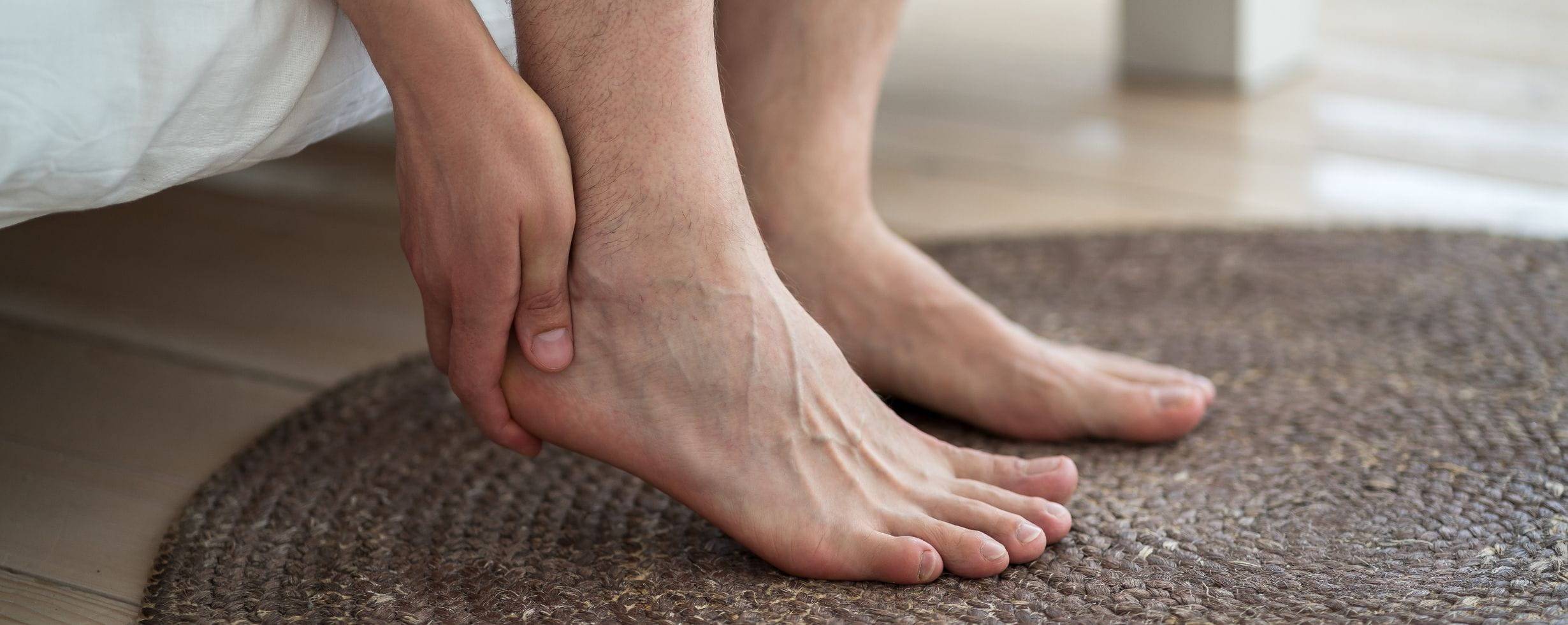
Experts explain plantar fasciitis, along with 7 ways to ease the pain – and how your most comfortable shoes may not be helping.

There’s a particular kind of pain that plantar fasciitis sufferers know all too well: a sharp, stabbing feeling under the heel with the first few steps out of bed or when you stand up after sitting for a while. It eases as you get moving, only to return with a vengeance later in the day.
If this sounds familiar, you’re in very good company. Plantar fasciitis is the most common cause of heel pain in adults, affecting roughly one in ten people over 50, according to research from Keele University. And while the instinct is to reach for the softest, most forgiving shoes in the wardrobe for some relief, that well-meaning choice might actually be part of the problem.
“Many people focus purely on cushioning, but overly soft or unsupportive footwear can actually increase strain by allowing the foot to collapse and work inefficiently,” says Jake Heath, sports podiatrist, director at the Royal College of Podiatry and founder of Foot Suite.
The plantar fascia is a thick band of connective tissue that runs along the sole of your foot, from the heel to the toes. Think of it as a kind of natural shock absorber, taking strain with every step. Plantar fasciitis is what happens when that tissue becomes irritated or develops small tears from being overloaded, often over months or even years.
“It’s less about a single injury and more about cumulative strain,” explains Dr Tony Banerjee of HarleyDoc. “Common contributors include prolonged standing, a sudden increase in activity such as running, tight calf muscles, poor foot biomechanics and inadequate footwear.”
The signature symptom is heel pain that is worst first thing in the morning or after a period of rest, easing with movement but creeping back as the day wears on.

If heel pain flares up in warmer months, your footwear is a prime suspect. Flip-flops, flat slides and those barely-there sandals we all reach for when the sun comes out offer almost no arch support or shock absorption and we tend to spend longer on our feet in summer, too.
“Flat, non-supportive sandals or worn-out shoes provide little arch support or shock absorption, which increases strain on the plantar fascia,” says Dr Banerjee. “Over time, especially if combined with long periods on your feet, this can contribute to the development or worsening of symptoms. It’s a very common trigger I see in clinical practice, particularly during warmer months.”
It’s not just flatness that’s the issue, either. As Heath points out, some sandals and “comfort” shoes prioritise squishy cushioning over structural support and that can create its own problems. The foot needs to be held and guided, not simply padded.
There’s a reason this condition turns up more often in middle age and beyond. Our feet, like the rest of us, change with time and not always in their favour.
“As we age, the plantar fascia becomes less elastic and less able to absorb shock,” explains Daniel Forbes, advanced paramedic practitioner and director of Forbes Medical Services. “There’s also often a reduction in the natural fat padding on the heel, which normally acts as a cushion. Combined with years of cumulative strain, especially in people who have spent a lot of time on their feet, this makes the tissue more prone to irritation and small tears.”
There’s another annoying issue as well. Once you’ve had plantar fasciitis, you’re more likely to get it again if the underlying causes aren’t addressed.
“Once the plantar fascia has been irritated or damaged, it can be more vulnerable to recurrence, particularly if things like poor footwear, tight calf muscles or reduced foot strength aren’t tackled,” Forbes says. “The key is not just treating the pain but correcting those contributing factors.”
The good news? Most cases improve with the right approach and there’s plenty you can do at home.
It’s worth knowing what doesn’t help when it comes to plantar fasciitis. Forbes highlights a handful of patterns he sees again and again:
Cushioning and support aren’t the same thing. A shoe that feels pillowy underfoot might still let your foot collapse inwards with every step, which is exactly what you don’t want.
“You want a shoe with good arch support, adequate cushioning, and a slight heel drop to reduce tension on the plantar fascia,” advises Dr Banerjee. “Trainers designed for stability or walking shoes are often ideal.”
If symptoms persist, orthotic insoles can be very helpful too. A podiatrist can advise on the right fit.
Kitchen tiles, wooden floorboards, slate hallways are all lovely to look at, but they are punishing for a sore heel. Padding around the house in bare feet or paper-thin slippers is one of the most common aggravators.
“Walking barefoot on hard surfaces is best avoided during recovery,” says Dr Banerjee. A pair of supportive indoor shoes or structured slippers can make a surprising difference.
Tight calves pull on the Achilles, which in turn tugs on the plantar fascia, so keeping them supple is one of the most effective things you can do.
“Tightness in the calves significantly increases the load through the plantar fascia,” explains acupuncturist Johnny Childs.
A simple standing calf stretch against a wall, held for 30 seconds on each side, two or three times a day, is a good starting point.

Childs recommends rolling the sole of the foot over a tennis ball to help release tension through the fascia. A frozen water bottle does the same job, adding a cooling, anti-inflammatory effect.
If you don’t have one to hand, simple pressure can be enough.
“Hold on any tender spots for 20 to 30 seconds to help release tension and improve circulation,” suggests Childs.
Do it while you’re watching television and you’ll barely notice the effort.
This might be the most underused tip on the list. Strong feet handle load better and building that strength is surprisingly simple. Towel scrunches (gathering a towel up with your toes) and heel raises (slowly rising onto tiptoes and lowering back down) take just a few minutes a day.
"Strengthening exercises for the foot and ankle can improve long-term resilience and reduce recurrence," says Dr Banerjee.
It’s tempting to rest up entirely when your heel is sore, but complete rest usually isn’t the answer.
“It’s about modifying rather than completely stopping,” says Dr Banerjee. “High-impact activities like running or jumping are often best reduced or paused temporarily, but low-impact exercise such as swimming or cycling can usually be continued and is encouraged to maintain overall fitness.”
The plantar fascia actually responds best to gradual, controlled loading, so staying active, within sensible limits, is part of the recovery, not separate from it.

Beyond rolling the foot, working firm pressure into the calf muscle itself can help ease the strain pulling on your heel.
“Using a massage ball or your hands to apply pressure into the middle of the calf can help relieve symptoms,” suggests Childs. “Consistency is key – gentle daily work is far more effective than occasional, intensive treatment.”
Some people also find acupuncture helpful alongside other measures. A 2017 review of clinical trials found that acupuncture may reduce plantar fasciitis pain in the short term, with benefits typically seen within four to eight weeks of treatment.
For many people, a few weeks of better footwear, daily stretching and gentle self-care is enough to settle symptoms, but if yours aren’t budging, don’t battle on alone.
“If symptoms persist beyond a few weeks despite simple measures, it’s worth seeking medical advice,” says Dr Banerjee.
“You should also consult a GP sooner if the pain is severe, worsening, or affecting your ability to walk.”
From there, further options such as physiotherapy, imaging, or a referral to a podiatrist can help and ruling out other causes of heel pain is always worthwhile.
The reassuring news is that plantar fasciitis is rarely a long-term problem when it’s handled properly. Supportive footwear – yes, even indoors – a little daily stretching and strengthening, plus a willingness to keep moving rather than retreat to the sofa will see most people right.
Perhaps the most important shift, though, is a mental one.
"Particularly in older adults, maintaining strength and movement quality is key” says Heath. “We should approach this more like training an athlete than managing a condition in isolation."
Your feet, which carry you through every single day of your life, will thank you for it.
(Hero image credit: GettyImages)
Jayne cut her online journalism teeth 25 years ago in an era when a dialling tone and slow page load were standard. During this time, she’s written about a variety of subjects and is just at home road-testing TVs as she is interviewing TV stars.
A diverse career has seen Jayne launch websites for popular magazines, collaborate with top brands, write regularly for major publications including Woman&Home, Yahoo! and The Daily Telegraph, create a podcast, and also write a tech column for Women’s Own.


Health insurance for people over 50 that provides a quicker route to diagnosis and planned medical treatment in a private facility.
Underwritten by Bupa Insurance Limited.

Click below for your chance to win a 15-night cruise to the Canary Islands on board Saga's Spirit of Adventure, worth more than £8,300.

Are you retiring at the wrong age? The best age to retire for your body, brain, happiness and pocket.


Everything you need to know about the lung infection, and how you could be ill with “walking” pneumonia without realising it.

Strong calves for a strong mind: how they support our circulation and brain health, with easy moves to strengthen yours at home.


Our GP Dr Mark Porter explains what can cause itchy skin, which is a common problem as we get older.

Worried you’ve morphed into Victor Meldrew? Find out how to battle that bad mood, and what to do if you’re stuck with a grouchy loved one.

The benefits of heat and cold therapy, and how Nordic bathing won over our nervous writer.

Here’s how to spot the symptoms of heat disease and reduce your danger.

The NHS winter vaccination campaign kicks off next week. Here’s the lowdown on what you need to book.

Pilates for back pain – what to do if you are suffering, and five gentle exercises that could help.

Dizziness or vertigo: a sensation of spinning, can stop us doing everyday things for fear of falling. Try these tips to stop feeling dizzy


You don’t have to put up with bladder leaks. We try out the latest pelvic floor gadgets for men and women.

Cataracts are a normal part of ageing. Learn how to spot the signs – and when it’s time to consider surgery.