Health & Wellbeing
Our experts show you simple and effective ways to stay healthy and active, so you can live your passions every day.

What your stride length says about your health
Could a short, uneven stride mean you could be at risk of future health problems?

New ways to prevent colds - and what worked for me
From supplements to sprays, can anything really stop that inevitable sniffle?

An insomniac’s guide to the best sleep aids
Our writer tried everything from pillows to trackers. But which worked best?

The 5 most common vitamin and mineral deficiencies as we age
Feeling tired or unsteady on your feet? You may be deficient in key vitamins and minerals.
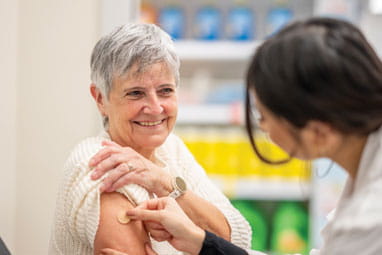
Your complete spring vaccinations guide
Covid, RSV and meningitis jabs - check your eligibility and which the experts say you should have.

Lower your blood pressure: 10 easy, natural ways
Medication can help, but you can also try these natural ways to lower your blood pressure.
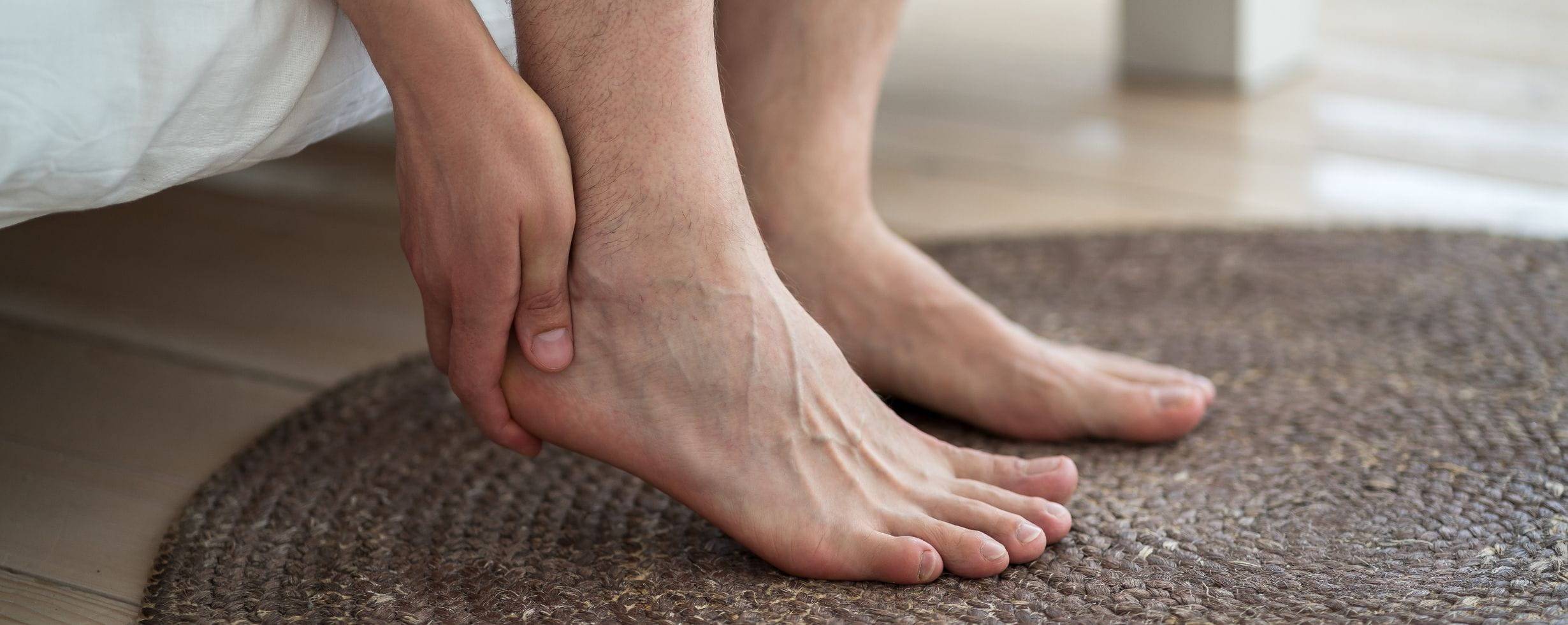
Plantar fasciitis: your summer shoes may be making it worse
Experts explain plantar fasciitis, along with 7 ways to ease the pain.

Is testosterone the key to vitality in later life?
Experts explain the pros and cons of testosterone replacement therapy.
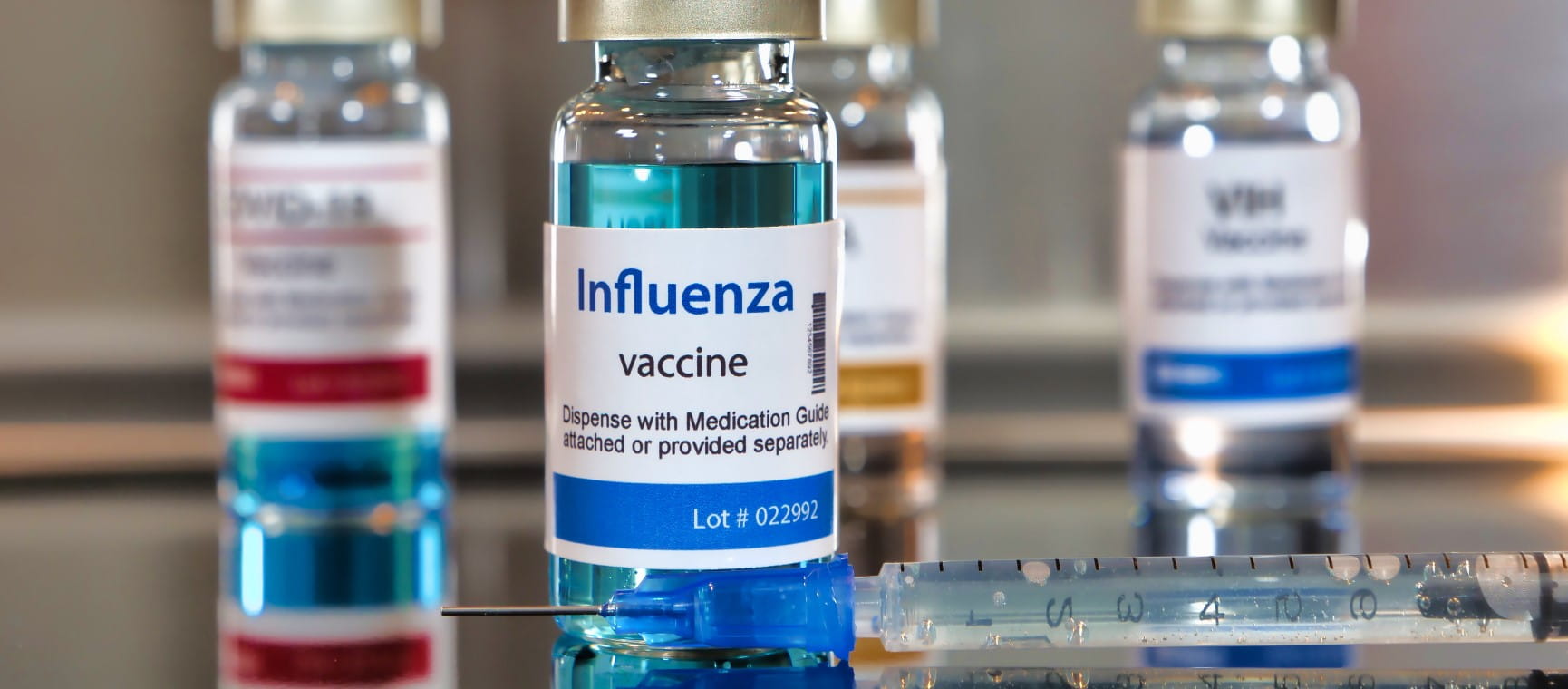
Which vaccines do you need this winter?
From flu to Covid to shingles, we answer common vaccine questions, including who’s eligible, and how you get them.

Should women over 70 be invited for regular mammograms?

Yeast intolerance diet tips
Find out what to stock your fridge with so you can avoid the bad breath, bloating, sugar cravings and other symptoms of yeast intolerance with our diet tips.

Your health in your hands - how they can reveal an underlying health condition
GP Dr Wendy Denning reveals the 13 changes in the way your hands look and feel that could be a sign of ill health.

Which nuts are healthiest? 6 of the best with benefits
Let’s roast the myths! Not only are nuts less fattening than once feared, research shows they can cut the risk of heart disease too.

Yoga for beginners – everything you need to know

This year, Saga is celebrating an incredible 75 years – and we’d love you to be part of the celebrations. For a limited time only, you can subscribe to Saga Magazine for just 75p an issue.
Receive the next 6 print editions delivered direct to your door, plus 6 months’ unlimited access to the Saga Magazine app – perfect for reading on the go.
Play our free daily puzzles
Beat the boredom and exercise your mind with our selection of free puzzles.





