Health & Wellbeing
Our experts show you simple and effective ways to stay healthy and active, so you can live your passions every day.

Do I need to take a magnesium supplement?
Do magnesium supplements really work – and how do you know if you’re getting enough?

Tea vs coffee: Which one is actually better for your health?
The experts brew up an answer and reveal the beverage benefits in full.
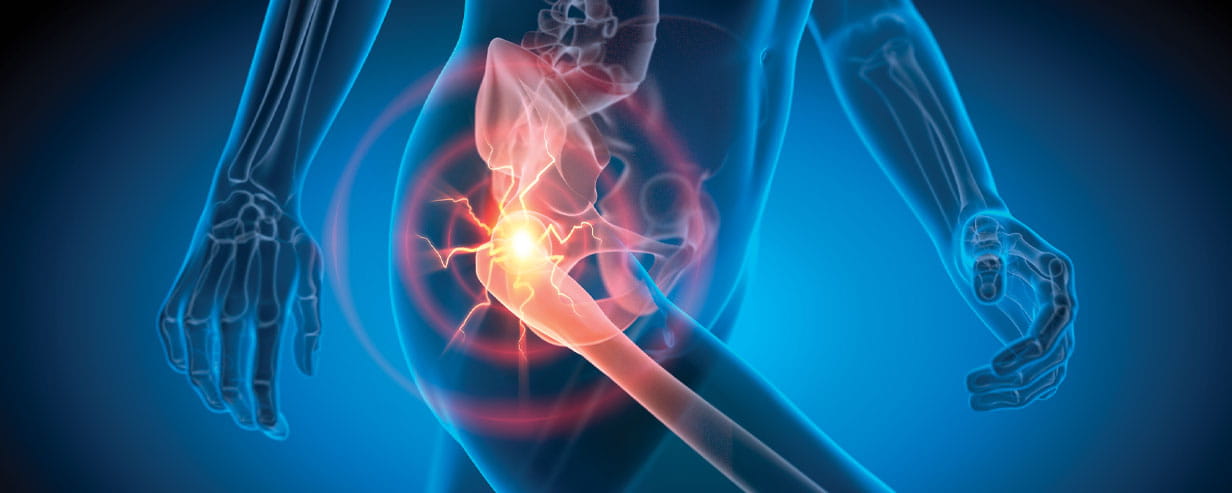
Expert ways to relieve the pain of dodgy hips
Try these tips and exercises to help you delay, or even prevent, a hip replacement.

How to live well with type 2 diabetes
The latest medical advice – from glucose monitors to oral health and lower carb diets.

What should I eat to keep my brain sharp?
5 surprising foods and drinks that could help your brain stay healthy as you age.
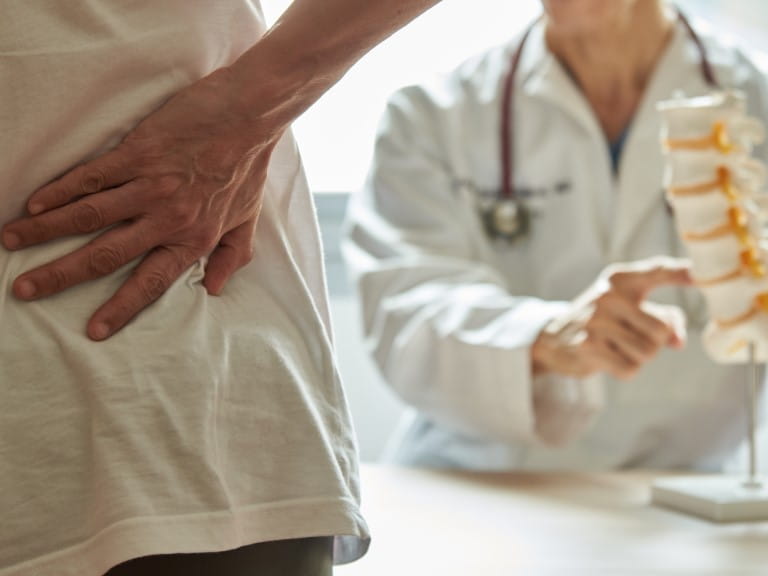
Back pain: These Pilates exercises could help
Pilates for back pain – what to do if you are suffering, and five gentle exercises that could help.

Jon Holmes: “How Stephen Fry saved my life”
The comedian on his prostate cancer and why he wants men to talk about health more.

Should I still take omega-3 supplements?
Expert advice on the latest research on the the benefits of omega-3.
9 expert ways to cut your chances of having a stroke
What steps can you take to minimise your stroke risk? Medical specialists offer their best advice.

7 healthy foods that could actually be bad for you

12 foods to boost testosterone naturally – and what to avoid
How can we naturally raise our falling testosterone levels as we age? Our experts have the answer

The healthiest ways to eat eggs
Poached, boiled or scrambled? We rank the best ways to eat eggs for your health.

Did mother really know best?
Which traditional health wisdoms still stand up and which belong firmly in the past?

Two surprising health drinks everyone should try
Staying hydrated is vital, but water isn’t the only answer, says wellness guru Liz Earle.

This year, Saga is celebrating an incredible 75 years – and we’d love you to be part of the celebrations. For a limited time only, you can subscribe to Saga Magazine for just 75p an issue.
Receive the next 6 print editions delivered direct to your door, plus 6 months’ unlimited access to the Saga Magazine app – perfect for reading on the go.
Play our free daily puzzles
Beat the boredom and exercise your mind with our selection of free puzzles.





