Health & Wellbeing
Our experts show you simple and effective ways to stay healthy and active, so you can live your passions everyday.

Are baked beans good for you? Health benefits and the best buys revealed

Do the new mood-boosting non-alcoholic drinks really work?
We test the latest functional booze-free drinks on the market to find the best and worst for taste and mood-boosting effect.

The unusual heart attack symptoms you need to know
Do you know the symptoms of a heart attack? Here’s what to look out for, and how to prevent one.

Dr Mark Porter on the pros and cons of weight-loss jabs for older people
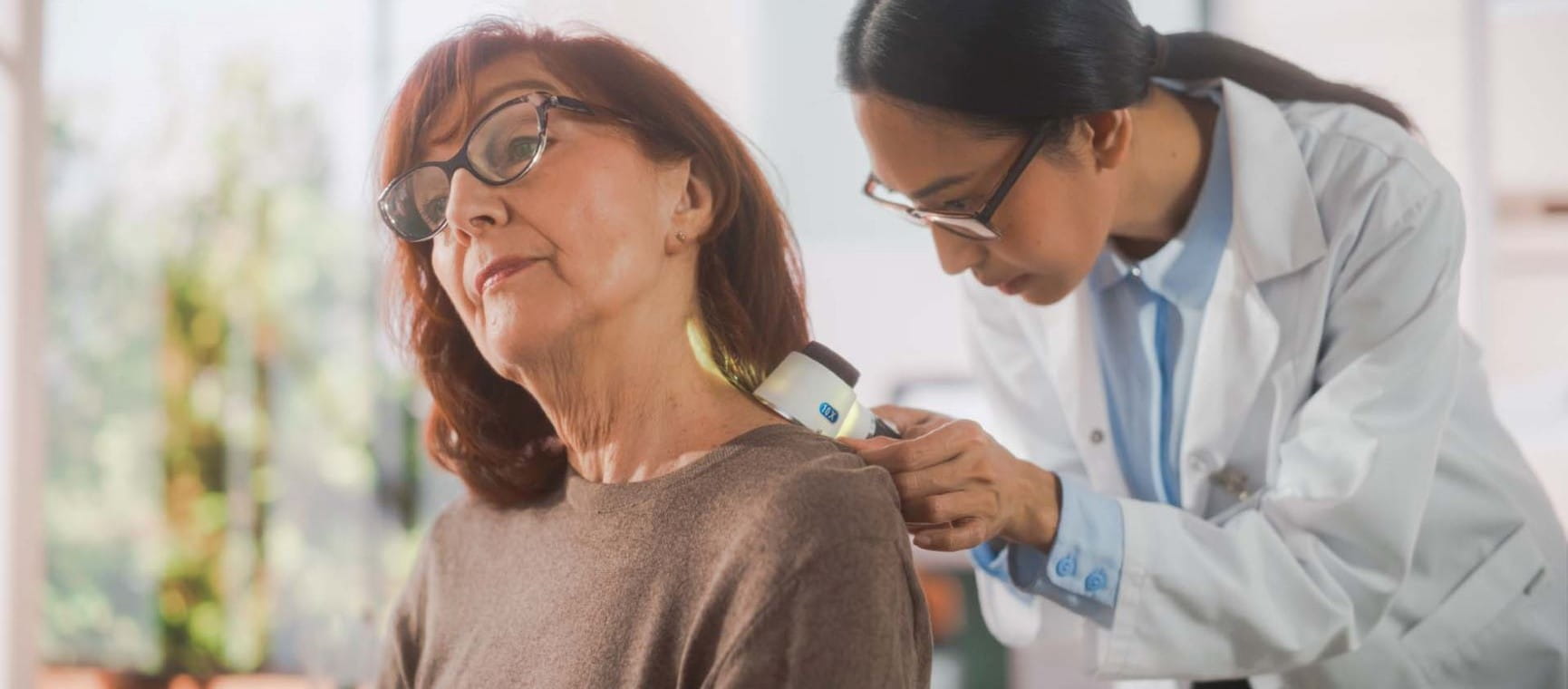
Skin cancer: what it looks like and how to minimise your risk
Our risk of skin cancer increases as we age. We explain the signs to look out for and why early treatment makes such a difference.

How to start exercising in later life

How many hours of sleep do I need as I get older?

7 ways to lower your cholesterol - naturally

What are white, pink and brown noise, and can they help your health?
You may know about white noise, but how about pink and brown noise? Learn their benefits.

Gout: all you need to know

Warning: the 9 everyday foods not to eat with medication
Our expert guide to the common foods you shouldn't mix with prescription drugs.

Sugar: should you give it up for your health?

The benefits of walking: is it the ultimate anti ageing exercise?
How walking can help you live longer, sleep better and even turn back the biological clock.

The healthiest fruits revealed, plus a few that aren’t worth the fuss

Perfect for browsing at home or on the go, the Saga Magazine app is packed with exclusive digital only content including interactive puzzles and games. You can even listen to some articles with our new audio feature.
Play our free daily puzzles
Beat the boredom and exercise your mind with our selection of free puzzles.



