Health & Wellbeing
Our experts show you simple and effective ways to stay healthy and active, so you can live your passions every day.
Your complete spring vaccinations guide
Covid, RSV and meningitis jabs - check your eligibility and which the experts say you should have.

The health benefits of chocolate

Is being too clean bad for your health?
We scrub, spray and sanitise our homes, but experts now say that dirt isn’t always the enemy.

Collagen: could it be the key to healthier joints and smoother skin?
Our experts explain the latest findings on the benefits of collagen in healthy ageing.

Our 10 best spring walks for wildflowers and views
Put a spring in your step with some of the best places to walk in the UK this season.

The best beginner yoga poses
Yoga is a great exercise for everyone. If you want to have a go, but don't know where to start, try our best beginner yoga poses

An insomniac’s guide to the best sleep aids
Our writer tried everything from pillows to trackers. But which worked best?

Lower your blood pressure: 10 easy, natural ways
Medication can help, but you can also try these natural ways to lower your blood pressure.

Gentle floor stretches for your lower back
Target stiffness and lower back tension with these simple and quick floor-based stretches.

The frozen foods that are healthier than fresh
Are we overlooking the nutritional benefits of frozen foods? Experts explain that some are actually better for you.

What your stride length says about your health
Could a short, uneven stride mean you could be at risk of future health problems?

Can ginger shots help my osteoarthritis?
GP Dr Mark Porter on whether ginger juice may calm inflammation.
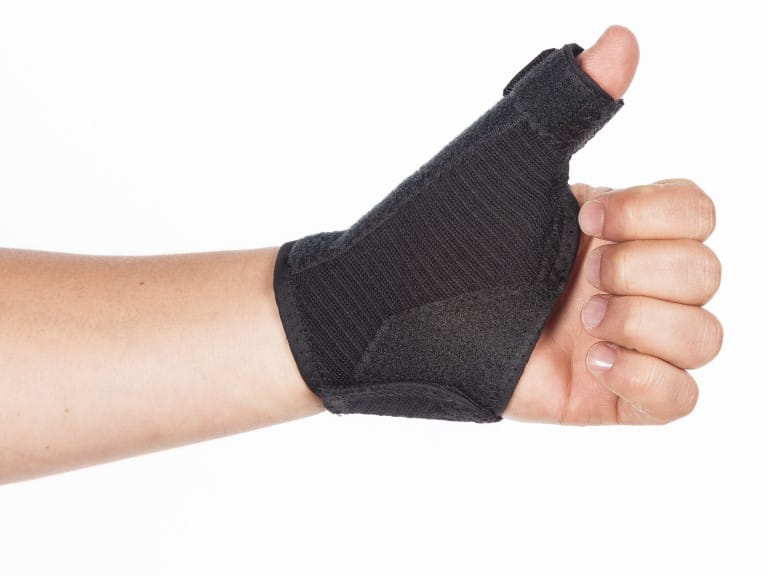
Can thumb splints help arthritis? Dr Mark Porter has the answer
What's the best way to deal with thumb arthritis

The hay fever mistake that could be making your symptoms worse
One of the most common ways to treat hay fever might actually be doing more harm than good.

This year, Saga is celebrating an incredible 75 years – and we’d love you to be part of the celebrations. For a limited time only, you can subscribe to Saga Magazine for just 75p an issue.
Receive the next 6 print editions delivered direct to your door, plus 6 months’ unlimited access to the Saga Magazine app – perfect for reading on the go.
Play our free daily puzzles
Beat the boredom and exercise your mind with our selection of free puzzles.





