Health & Wellbeing
Our experts show you simple and effective ways to stay healthy and active, so you can live your passions every day.

Can what you eat slow ageing? A neuroscientist says yes
Dr David Cox explains the link between our diet and how we age.

AI glasses could transform life for those with dementia
Specs that help wearers find the right words and do basic tasks are to be trialled this autumn.
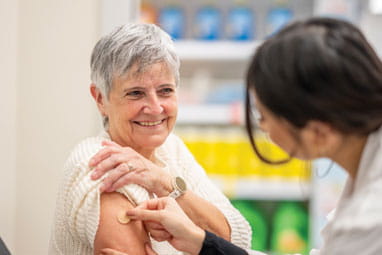
Your complete spring vaccinations guide
Covid, RSV and meningitis jabs - check your eligibility and which the experts say you should have.

The 5 drinks that could be keeping you awake
Experts explain the drinks that could be stopping you sleeping, with simple swaps for a restful night.

The hay fever mistake that could be making your symptoms worse
One of the most common ways to treat hay fever might actually be doing more harm than good.
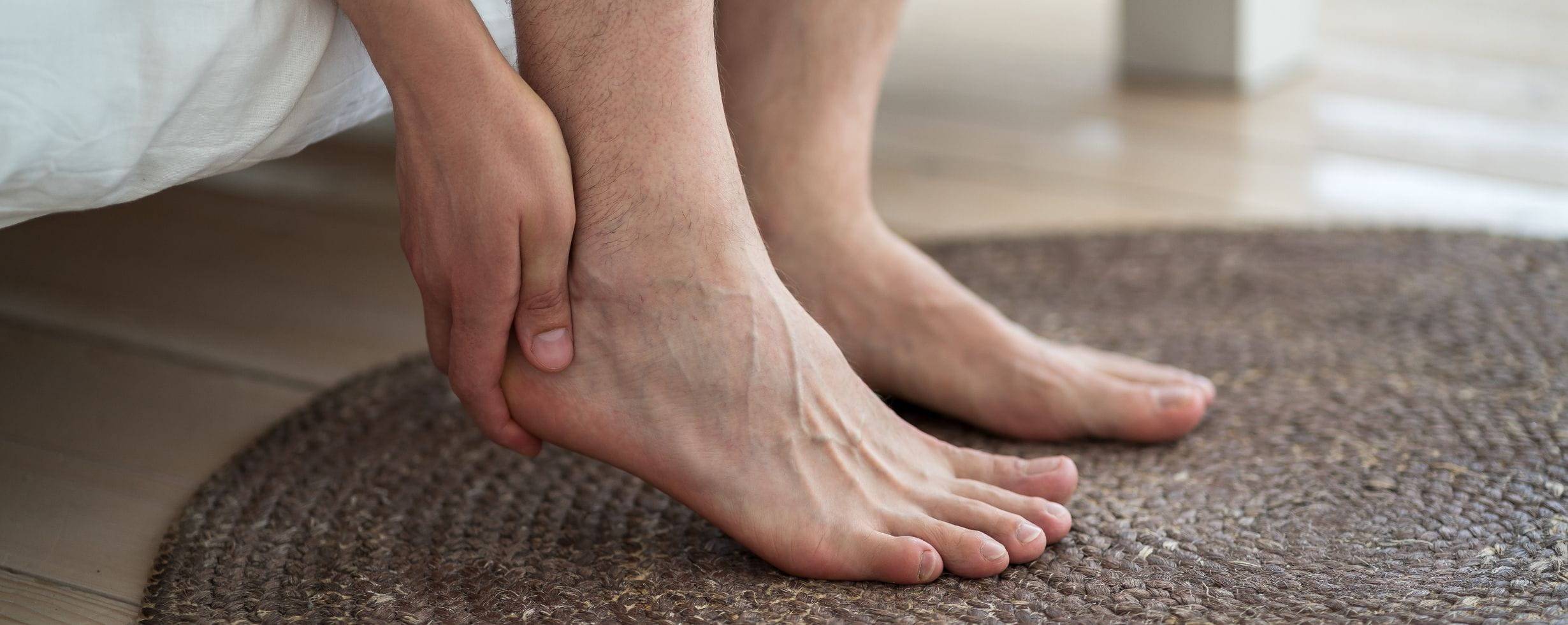
Plantar fasciitis: your summer shoes may be making it worse
Experts explain plantar fasciitis, along with 7 ways to ease the pain.

What are ultra-processed foods and how to cut back

AI glasses could transform life for those with dementia
Specs that help wearers find the right words and do basic tasks are to be trialled this autumn.
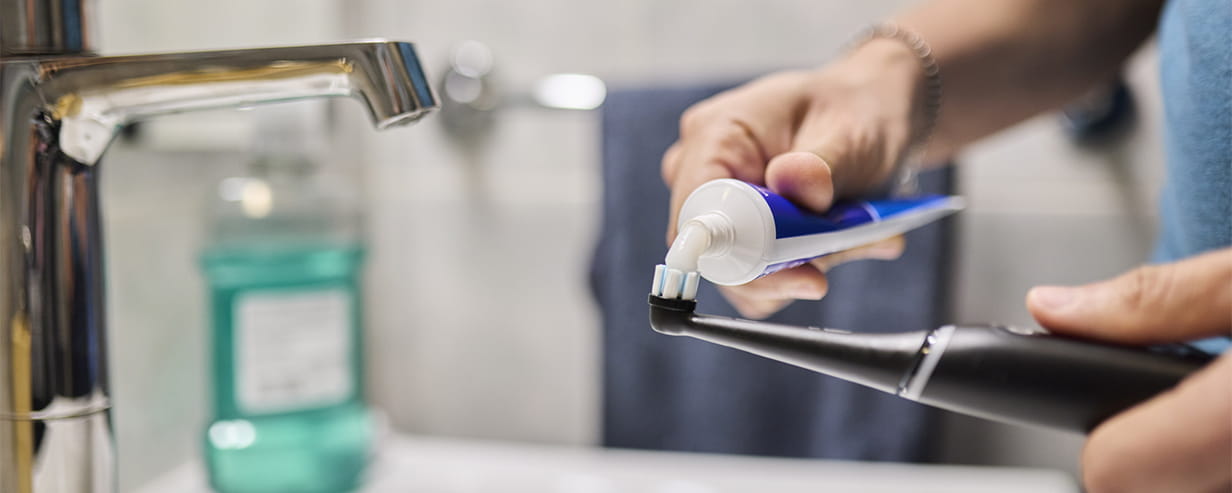
How taking care of your teeth and gums help could stave off dementia
Poor oral hygiene could raise our risk of more than 50 diseases, including dementia and arthritis.

Plantar fasciitis: your summer shoes may be making it worse
Experts explain plantar fasciitis, along with 7 ways to ease the pain.

These foods can ease everyday pain
The 3 common ailments to which diet changes can really make a difference.

Can what you eat slow ageing? A neuroscientist says yes
Dr David Cox explains the link between our diet and how we age.

Is testosterone the key to vitality in later life?
Experts explain the pros and cons of testosterone replacement therapy.

New ways to prevent colds - and what worked for me
From supplements to sprays, can anything really stop that inevitable sniffle?

This year, Saga is celebrating an incredible 75 years – and we’d love you to be part of the celebrations. For a limited time only, you can subscribe to Saga Magazine for just 75p an issue.
Receive the next 6 print editions delivered direct to your door, plus 6 months’ unlimited access to the Saga Magazine app – perfect for reading on the go.
Play our free daily puzzles
Beat the boredom and exercise your mind with our selection of free puzzles.





