Health & Wellbeing
Our experts show you simple and effective ways to stay healthy and active, so you can live your passions every day.
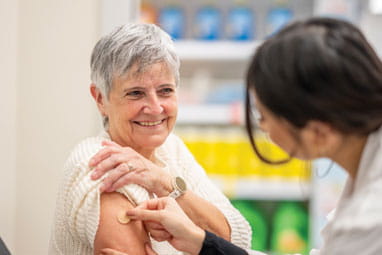
Your complete spring vaccinations guide
Covid, RSV and meningitis jabs - check your eligibility and which the experts say you should have.

The health benefits of chocolate

Is being too clean bad for your health?
We scrub, spray and sanitise our homes, but experts now say that dirt isn’t always the enemy.

Collagen: could it be the key to healthier joints and smoother skin?
Our experts explain the latest findings on the benefits of collagen in healthy ageing.

Our 10 best spring walks for wildflowers and views
Put a spring in your step with some of the best places to walk in the UK this season.

The best beginner yoga poses
Yoga is a great exercise for everyone. If you want to have a go, but don't know where to start, try our best beginner yoga poses

Can keeping the curtains open improve your sleep?
We find out whether waking up to natural light really helps you sleep better.

Exercise and menopause – what you need to know
Expert advice to help you keep healthy and active during and after the menopause.

A new study suggests the shingles vaccine can protect against dementia - should you have it?
Two experts on whether the jab does make a difference - and what else you can do to protect yourself.

Could your morning fruit juice be raising your cancer risk?
Our nutrition experts share the best and worst juices for your health – and they might surprise you.

Couch to 5k: why you should start and how to keep going
Get up and running with couch to 5k.

The health benefits of chocolate

Our 10 best spring walks for wildflowers and views
Put a spring in your step with some of the best places to walk in the UK this season.

Your complete spring vaccinations guide
Covid, RSV and meningitis jabs - check your eligibility and which the experts say you should have.

This year, Saga is celebrating an incredible 75 years – and we’d love you to be part of the celebrations. For a limited time only, you can subscribe to Saga Magazine for just 75p an issue.
Receive the next 6 print editions delivered direct to your door, plus 6 months’ unlimited access to the Saga Magazine app – perfect for reading on the go.
Play our free daily puzzles
Beat the boredom and exercise your mind with our selection of free puzzles.





